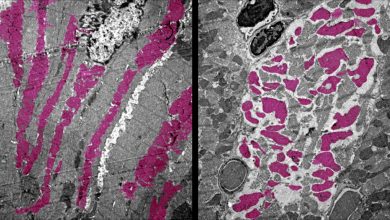
Researchers in the US have developed a new multi-organ-on-a-chip to test how new drugs affect the human body’s vital organs.
Developing new drugs can come at an enormous financial cost, which can be wasted if the drug must be withdrawn due to unforeseen side effects.
The research team believes their new system – containing representations of liver, heart, vasculature, lungs, testis, and either colon or brain tissues – could help avoid such cases.
In their study, published in the journal Biofabrication, they demonstrated its effectiveness by using it to screen a selection of drugs that were recalled from the market by the US Federal Drug Administration (FDA).
Professor Anthony Atala, from the Wake Forest Institute for Regenerative Medicine (WFIRM), Winston-Salem, US, is the study’s senior author. He said: “The development of new drugs can take a decade and a half, from preclinical studies to reaching the market. Around one in 5,000 drug candidates successfully completes this journey. Additionally, the cost for bringing a single drug to market, with all direct and indirect expenses accounted for, can climb as high as $2.6 billion.
“Unfortunately, the human and financial costs can be even more dramatic if a drug is later found to be harmful and must be withdrawn. For example, Merck & Co. paid $4.85 billion to settle 27,000 cases and another $830 million dollars to settle shareholder lawsuits after one of its drugs caused adverse effects. The human costs of adverse drug reactions, meanwhile, manifest themselves as a leading cause of hospitalization in the United States, with up to 5.3 percent of hospitalizations related to adverse drug reactions. The rate of fatal adverse drug reactions is difficult to determine, and it is probably underreported. As both adverse human effects and drug development costs increase, access to more reliable and affordable drug screening tools is increasingly critical.”
Co-author Dr. Aleksander Skardal, formerly of WFIRM and now at Ohio State University, said: “This increasing need to comprehensively screen new drugs for adverse effects is the driving force behind our research. In this context, we demonstrated our platform by screening a panel of FDA-recalled drugs for toxic effects.
“To model the integrated nature of the human body, we designed an integrated platform, or chip, supporting six tissue types under a common recirculating media. When combinations of organoids are combined into a single platform, more complex integrated responses can be seen, where the functionality of one organoid influenced the response of another.”
To test their system, the researchers used it to screen six drugs that had been recalled due to adverse effects in humans: pergolide, rofecoxib, valdecoxib, bromfenac, tienilic acid and troglitazone. For many of these compounds, the 3D organoid system was able to demonstrate toxicity.
Professor Atala said: “These compounds were tested by the pharmaceutical industry and toxicity was not noted using standard 2D cell culture systems, rodent models, or during human Phase I, II and III clinical trials. However, after the drugs were released to the market and administered to larger numbers of patients, toxicity was noted, leading the FDA to withdraw regulatory approval. In almost all these compounds, the 3D organoid system was able to readily demonstrate toxicity at a human-relevant dose.”
As a control, they also tested the system with commonly-used drugs still on the market – aspirin, ibuprofen, ascorbic acid, loratadine, and quercetin. As well as not showing any toxicity, the organoids exposed to these non-toxic compounds remained viable at clinically-relevant doses.
Dr. Skardal said: “Further study will be needed. But based on these results our system, and others like it, using 3D human-based tissue models with nuanced and complex response capabilities, has a great potential for influencing how in-vitro drug and toxicology screening and disease modelling will be performed in the near future.”