A team of researchers has proven that the composition of immune cells that are found to infiltrate primary prostate tumors are determined by genetic variation causing prostate cancer
Cancer Immunotherapy is the treatment also known as biological therapy in which immune system is used to fight cancer. This therapy helps the immune system to work fully to destroy cancer cells.
The field of immunotherapy is significantly changing the cancer treatment nowadays. Yet clinical trials often show noticeable progress only in a small group of patients. this shows that there is an unidentified difference among tumors which is leading to diverse paths of disease development and response to therapy.
A team led by the researchers at the Cancer Center at Beth Israel Deaconess Medical Center (BIDMC) have proven that the composition of immune cells that are found to infiltrate primary prostate tumors are determined by genetic variation causing prostate cancer. These immune cells, in turn, direct the tumor progression and reaction to treatment.
The data, published in Nature Medicine, suggest that profiling patients’ tumors based on this new information could lead to more successful clinical trials and tailored therapies for patients. “We observed that specific genetic events resulted in striking differences in the composition of immune cells present in and around the tumor – results with important therapeutic implications,” said senior author Pier Paolo Pandolfi, MD, Ph.D., Director of the Cancer Center and Cancer Research Institute at BIDMC. “Our data may be especially relevant for tailoring immunological therapies and for identifying the responsive-patient population.”
In Prostate cancer, the prostate gland, which produces some of the fluid in semen and plays a role in urine control in men gets affected. in the U.S., It is the third leading reason for cancer-related death in men, prostate cancer, is linked to a number of diverse genetic mutations that drive the disease.
For example, in prostate cancer, PTEN, tumor suppressor gene get which in turn promote the disease in combinations with a plethora of other mutations. Researchers also found that tumor progression and response to therapy are also affected the tumor’s microenvironment like the immune cells, blood vessels, signaling molecules and other factors that surround the tumor.
In the laboratory, a team of researchers engineered the mice models and represented the four distinct known genetic variations of human prostate cancer. Pandolfi’s team – including lead author, Marco Bezzi, a post-doctoral fellow in Pandolfi’s lab. The models lacked either Pten alone or in combination with other genetic alterations known to drive the disease. After analyzing these mice models for tumor, they found that there are intense differences in the type of immune cell around the tumor as well as the number of immune cells produced in surrounding of the
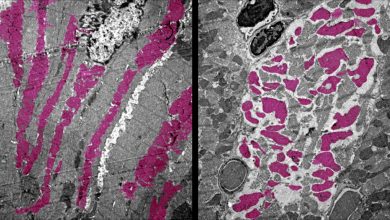
They further added, they noticed an increased accumulation of myeloid cells in the specific immune landscapes tumors of the genetic model that lacked both Pten and the tumor suppressor gene called Trp53. myeloid cells are the immune cells that mediate immunosuppression. In contrast to these genetic model lacking Pten and a different tumor suppressor gene called PML lacked intratumoral immune infiltration. In these tumors, the scientists found no immune cells at all, which dubbed “cold,” or “immune-deserts.” On analyzing all the four mouse models, researchers concluded that all were showing different immune landscapes and these differences were maintained and were worsened over time.
The scientist also showed that genetic variation which led to tumor was directly controlling the differences in the composition of immune cells. They also observed that different tumors were secreting different chemical attractants which lead to recruitment of different immune cell in some tumors and no recruitment in others like in immune desert tumors. They also added that these genetic variations hold true in human prostate cancer and for growth and progression of these tumors, recruitment of immune cells is important.
According to the one of the author Bezzi, “by blocking the recruitment of infiltrating immune cells, tumor growth can be inhibited. In the light of this effective therapies can be found for blocking the specific immune landscapes. “On the other hand, the cancer genotype characterized by the so-called ‘immune desert’ phenotype, did not respond to such therapies. On this basis of this finding, we can anticipate the tumor response to immunotherapies and modify treatment modalities to efficiently influence tumors that are otherwise extremely destructive,” he said.
These new discoveries can be used to find the more effective and precise combinations of immunotherapies which can be used to target tumor on the basis of the different cancer genetic makeup.
“These profound differences in immunological landscapes among various cancer genotypes further highlight the need to thoroughly investigate and integrate genotypes and immune-phenotypes in the context of exploratory cancer treatments in both preclinical and clinical settings,” said Pandolfi.